FLEA-RELATED DERMATITIS
Fleas are, directly and indirectly, probably the cause of more dermatological disorders in small animals than all other etiological agents together. Flea allergy dermatitis (FAD), or flea-bite-hypersensitivity, is the most common small animal dermatological condition (Cole, 2008; Dryden, 2009; Scott et al., 2001), making appropriate flea control indispensable.
FAD is a hypersensitive state induced in the host by injection of salivary antigens at the time of flea feeding. In cats and dogs with FAD, flea bites cause mechanical irritation, annoyance and pruritus (Siak & Burrows, 2013).
Generally, once the flea has found a host for the uptake of blood, a few test bites are performed until a blood leading capillary vessel has been found (Karandikar and Munshi, 1950). The direct contact with the host’s skin as well as these bites have shown to cause an irritation of the skin, pruritus and an insignificant, transient invasion of lymphocytes in the direct proximity of the biting site (Gothe, 1985). This reaction seems to be caused by the direct contact of the skin with the ectoparasite and its bite.
Flea saliva contains histamine-like compounds, proteolytic enzymes, and anticoagulants. These proteins are released into the host during feeding and can act as inflammatory or antigenic stimuli in sensitive animals (Lam and Yu, 2009). Various immunologic responses are provoked, including immediate (type I) and/or delayed (type IV) hypersensitivity reactions (Bond, 2014; Gross and Halliwell, 1985), late-phase IgE-mediated responses, and cutaneous basophil hypersensitivity reactions (Halliwell et al., 1987).
The main clinical sign in FAD is pruritus. Alopecia, crustiness and the flea bite itself as well as pustules and papules can further be observed. In dogs, clinical signs often manifest on the caudal aspect of the animal (Lam and Yu, 2009). Self-induced alopecia, erythema, pyotraumatic dermatitis, dull, coarse haircoat, hyperpigmentation and/or lichenification may be observed (Scott et al., 2001). In cats, dorsal lumbosacral pruritus with miliary dermatitis is noted most commonly with flea bite hypersensitivity (Hobi et al., 2011), but other reaction patterns may also be observed in the feline patient, including eosinophilic plaques or ulcers, bilaterally symmetrical self-induced alopecia, ventral abdominal alopecia, or generalized pruritus (Hobi et al., 2011).
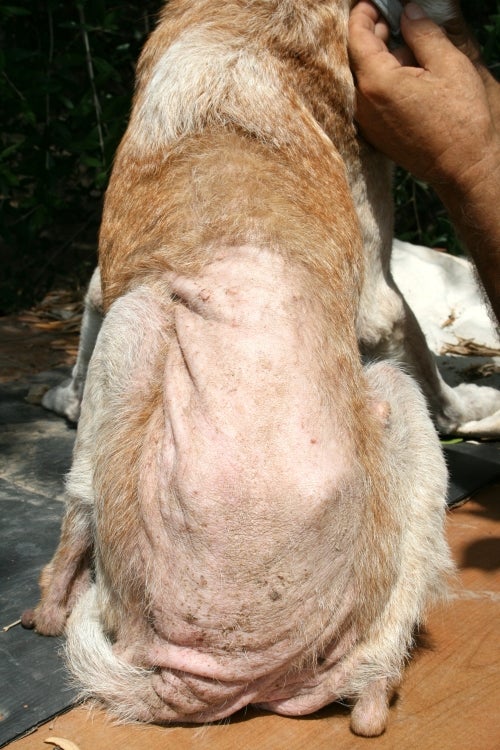
Dog showing flea allergic dermatitis (FAD) with massive self-induced alopecia and lichenification, especially in the caudal dorsum
Traditionally, it was believed that a single flea bite was sufficient to cause the clinical signs of FAD. More recently, the concept of a ‘pruritus threshold’ has been introduced, which suggests that (here) cats can tolerate a certain pruritic load without demonstrating clinical signs and that pruritus is only initiated if this threshold level is breached (Siak and Burrows, 2013). FAD is likely to be dependent on the degree of hypersensitivity of the host, the total flea burden and the amount of flea antigen injected during flea feeding (Siak and Burrows, 2013).
Irrespective, whether a few or even a single flea bite is sufficient to start an allergic reaction, a rapid, ideally complete reduction and elimination of the total flea numbers and a decrease, ideally a total prevention of flea feeding are essential and are the keys to controlling the clinical signs of FAD.
References
Bond R: Pathogenesis (Flea Bite Allergy). In: Noli C, Foster A, Rosenkrantz W (eds.): Veterinary Allergy. 2014, Wiley Blackwell, West Sussex, UK, pp. 249-51
Cole LK: Fleas and flea allergy dermatitis. 6th Proc World Congr Vet Dermatol. 2008, pp. 119-25
Dryden MW: Flea and tick control in the 21st century: challenges and opportunities. Vet Dermatol. 2009, 20, 435‐40
Gothe R: [Pathogenesis of arthropod infestations.] Berl Münch Tierärztl Wochenschr. 1985, 98, 274-9 [in German]
Halliwell RE, Preston JF, Nesbitt JG: Aspects of the immunopathogenesis of flea allergy dermatitis in dogs. Vet Immunol Immunopathol. 1987, 17, 483-94
Hobi S, Linek M, Marignac G, et al.: Clinical characteristics and causes of pruritus in cats: A multicentre study on feline hypersensitivity-associated dermatoses. Vet Dermatol. 2011, 22, 406-13
Karandikar KR, Munshi DM: Life history and bionomics of the cat flea, Ctenocephalides felis felis (Bouché). J Bombay Nat His Soc. 1950, 49, 169-77
Lam A, Yu A: Overview of flea allergy dermatitis. Compend Contin Educ Vet. 2009, 31, E1‐E10
Scott DW, Miller WH, Griffin CE: Skin immune system and allergic skin disorders. In: Scott DW, Miller WH, Griffin CE (eds.): Muller and Kirk’s Small Animal Dermatology. 6th edn., 2001, WB Saunders, Philadelphia, USA, pp. 543-666
Siak M, Burrows M: Flea control in cats: new concepts and the current armoury. J Feline Med Surg. 2013, 15, 31-40
EXPLORE OUR CONTENT
 CVBD MapsThe CVBD Occurence World Map presents country-specific situations based on current scientific knowledge and feed-back from experts around the world in an easy-to-grasped way. |
| Read more-> |
 ResourcesElanco Animal Health supports education in parasitology and especially in the field of vector-borne diseases. Access image collections, discover the World Forum calendar, interesting links and our glossary. |
| Read more-> |
 CVBD World ForumThe CVBD World Forum is a working group of leading international experts with the mission to enhance knowledge and communication on companion animal vector-borne diseases for the improvement of animal, human, and environmental health. |
| Read more-> |
